Why this lung cancer returns—and why inflammation may be key
Why this lung cancer returns—and why inflammation may be key📷 Published: Mar 27, 2026 at 18:12 UTC
- ★Protein loss fuels tumor growth via inflammation
- ★Cancer cells shift to neuron-like, aggressive state
- ★No immediate patient impact—but a clear research target
Small cell lung cancer kills 95% of patients within five years, often because it returns after treatment. Now, scientists have identified a critical piece of that puzzle: the loss of a still-unnamed protein triggers inflammation that doesn’t fight the tumor—it feeds it. Published in ScienceDaily Health, the research confirms that this inflammatory response does more than promote growth; it pushes cancer cells into a neuron-like state linked to relapse.
The finding is precise but preliminary. This isn’t a discovery of a new drug or even a biomarker for clinical use. It’s a mechanistic insight, observed in lab models, showing how a protein’s absence rewires the tumor microenvironment. The aggression of these neuron-like cells isn’t just theoretical: prior studies, like those in Nature Cancer, have tied such cellular shifts to treatment resistance in other cancers.
Yet the study’s limits are as important as its breakthrough. The protein itself remains unnamed in public reports, and the work appears to rely on preclinical models—not patient samples or clinical trials. That gap matters: what holds true in a petri dish or mouse model often falters in human biology.
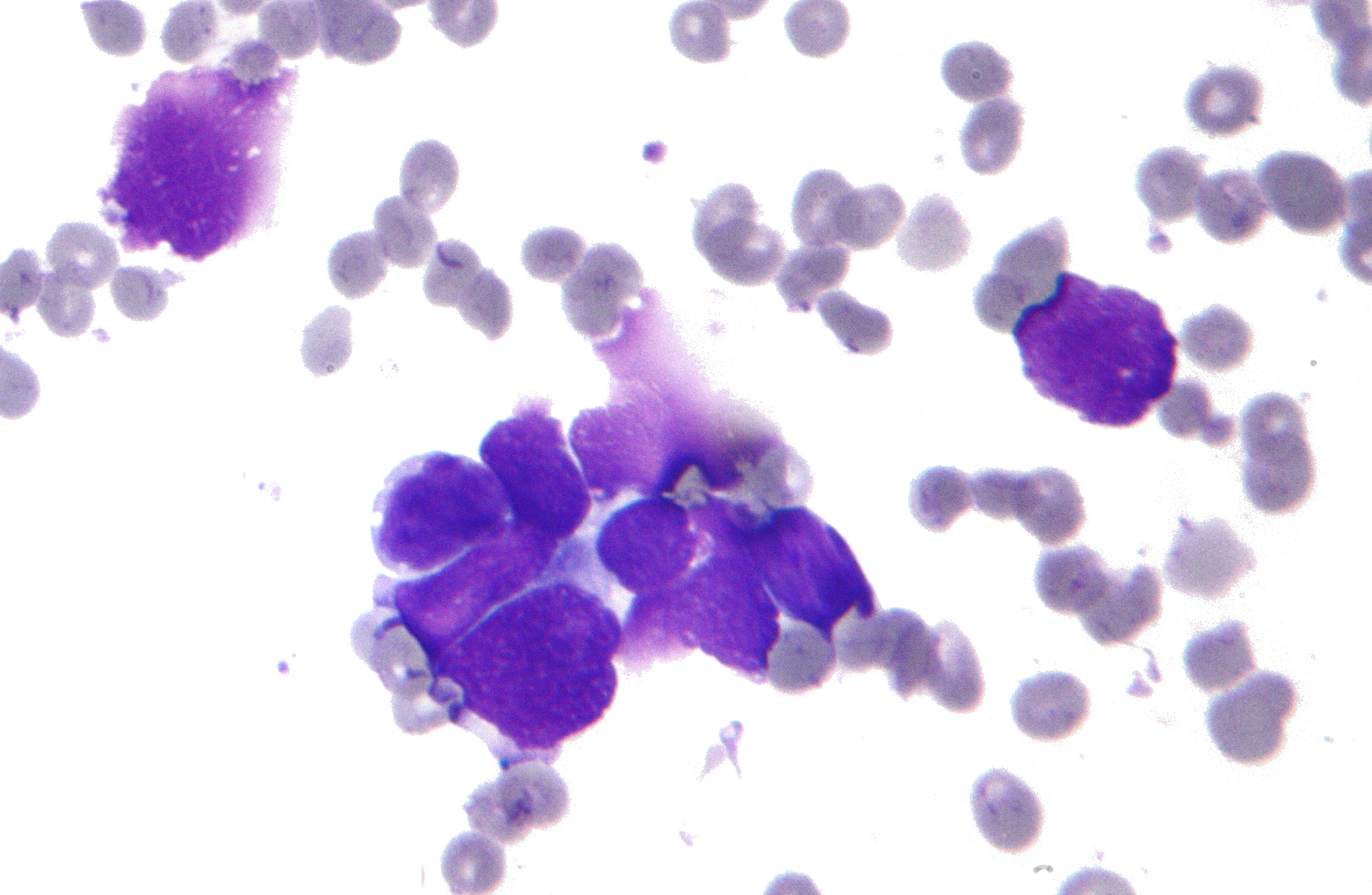
A molecular trigger found, but the clinical path remains long📷 Published: Mar 27, 2026 at 18:12 UTC
A molecular trigger found, but the clinical path remains long
For patients today, this changes nothing. No new tests, no altered treatment protocols. The real value lies in the research roadmap it provides. If this protein pathway is confirmed in human tumors, it could become a target for therapies that block the inflammatory feedback loop—or even reverse the neuron-like transformation. But that’s a series of ifs stacked on years of validation.
The clinical bottleneck isn’t scientific ignorance; it’s translation. Small cell lung cancer’s lethality stems from its rapid evolution, and this study underscores how deeply that evolution is tied to the immune system’s misfiring. Yet the history of cancer research is littered with promising molecular targets that failed in trials. The NCI’s own reviews caution that even well-understood pathways rarely yield quick wins.
What’s missing? First, the protein’s identity—without it, designing inhibitors is impossible. Second, proof that disrupting this inflammation in humans doesn’t trigger worse side effects. And third, data on whether neuron-like cells in patients behave like those in the lab. Until then, this remains a compelling hypothesis, not a clinical tool.
The critical unanswered question isn’t whether this pathway exists, but whether it’s druggable without collateral damage. And that’s a question only human trials can answer.